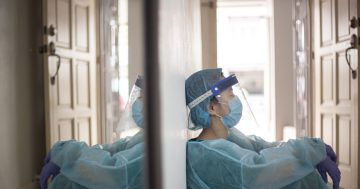
An independent expert inquiry has alleged that the United Kingdom Government’s reliance on private sector contracts at the expense of existing public structures and expertise is a key reason for the country’s high pandemic death rate.
An independent expert inquiry has alleged that the United Kingdom Government’s reliance on private sector contracts at the expense of existing public structures and expertise is a key reason for the country’s high pandemic death rate.
In its interim conclusions, the informal People’s COVID Inquiry said a decade of savage austerity policies had left the National Health Service (NHS), social care, and other public services understaffed, weakened, and insufficient.
It considered the lack of any Government-commissioned inquiry into the United Kingdom’s response to the pandemic a “stark dereliction of public duty” that could breach national and international legal obligations.
Professor of Neonatal Medicine at Imperial College London and a panellist on the inquiry, Neena Modi said that instead of investing in the NHS, the pandemic had been used to underwrite the private healthcare sector with public funds.
“Captain Tom, the centenarian who walked his garden again and again to raise £39 million ($A72.5 million) for the NHS, would have been appalled to have realised that money has been wasted on a failed test-and-trace system,” Professor Modi said.
“These actions have left public services even weaker and even less prepared,” she said.
The inquiry, chaired by human rights barrister, Michael Mansfield was convened by the campaign group Keep Our NHS Public.
It has heard evidence from 39 experts, key workers, patients, and bereaved people over nine hearings since February.
Interim recommendations include calls for the urgent implementation of proven public health measures such as testing, contact tracing, and support for people to isolate, instead of an over-reliance on vaccines.
It said the Government should also implement long-term policies to reduce widening social inequalities that drive health inequalities, consider health in all policies, and bring forward new regulations to improve ventilation in enclosed spaces like schools and workplaces.
The inquiry called for funding in public care systems to include not only hospital beds but also the workforce, primary care, diagnostic capacity, social care, and public health.
The inquiry’s final conclusions are expected in the autumn.
London, 10 July 2021